Neurofibromatosis Type 2
Definition and Clinical Features
|
As with NF1 Opens in new window, NF2 is autosomal dominant, has a high degree of penetrance Opens in new window, and is characterized by acoustic neuromas. Neurofibromatosis type 2 (NF2) is a multisystem disorder with prominent features of central nervous system tumors including bilateral vestibular schwannomas (acoustic neuromas), spinal cord schwannomas, meningiomas, gliomas, and juvenile posterior subcapsular cataract. |
Neurofibromatosis type 2 is also referred as MISME syndrome, a mnemonic referring to related tumors of MIS (multiple inherited schwannomas), M-meningiomas, and E-ependymomas. Cutaneous features are less often seen with this form of neurofibromatosis.
Neurofibromatosis type 2 can be associated with reduced life span secondary to central nervous system tumors, particularly if they are present at a young age and are multiple.
The average age at symptom onset is approximately 20 years but can be delayed. Early age at symptoms and the presence of intracranial meningioma at diagnosis are two signs of higher risks for disease severity and mortality.
The incidence of neurofibromatosis type 2 is 1 in 25000 live births and has nearly 100% penetrance by 60 years of age. NF2 is related to a mutation in the NF2 gene at chromosome 22q12.2. This gene produces merlin (also called neurofibromin-2), a tumor suppressor. When mutated, decreased function of merlin leads to the uncontrolled development of tumors, particularly in the central nervous system. One-half of affected patients have a de novo mutation.
Ophthalmologic Features
Neurofibromatosis type 2 displays three important ophthalmologic findings, notably posterior subcapsular cataract in childhood, combined hamartoma of the retina and retinal pigment epithelium, and epiretinal membranes.
The juvenile posterior subcapsular cataract (<50 years) is a criterion for diagnosis of this condition. Other lens opacity in the capsular or cortical region of young patients are believed related to neurofibromatosis type 2. Lisch nodules are not a feature of neurofibromatosis type 2.
Epiretinal membranes and combined hamartoma of the retina and retinal pigment epithelium can have overlapping clinical phenotype and can be multifocal.
Of those with severe clinical features of neurofibromatosis type 2, 80% display epiretinal membranes. The hamartomas are along the inner retina but lead to prominent retinal dragging, corkscrew retinal vessels, gray-green appearance and tumor formation.
Dermatoogic Features
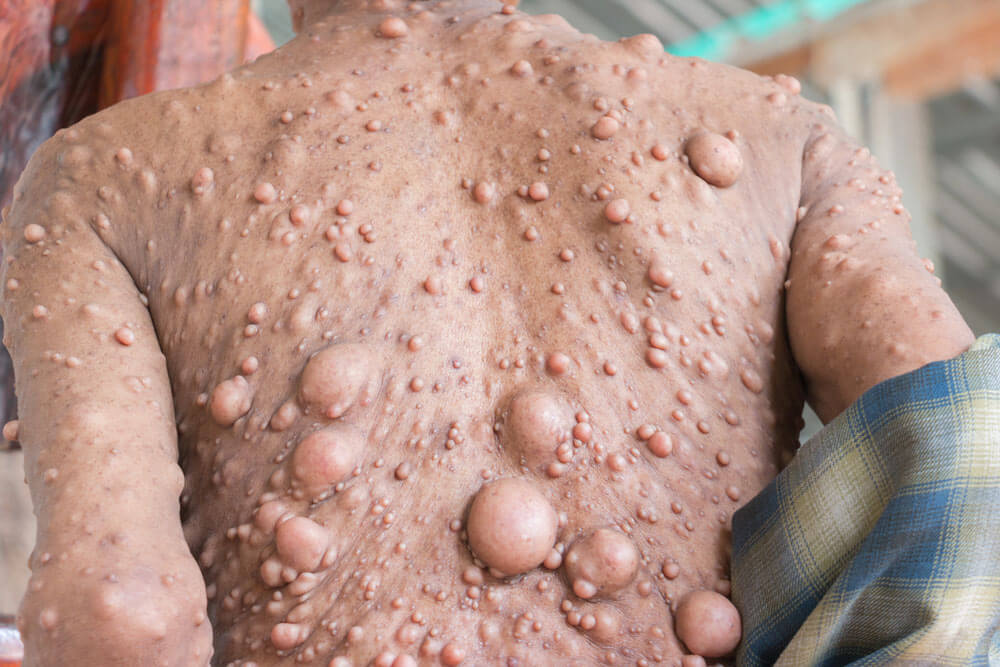
The cutaneous features of neurofibromatosis type 2 are slightly different than those in type 1. Occasionally, overlap of the two conditions can be seen. Café-au-lait spots are occasionally found. Axiallary or inguinal freckling is not often found with neurofibromatosis type 2.
Subcutaneous schwannomas or neurofibromas can be found and malignant transformation is extremely rare. Neurofibromatosis type 2 displays skin plaques, represented by well-circumscribed, roughened areas less than 2 cm and often with slight hyperpigmentation and hypertrichosis.
Central Nervous System Features
Neurofibromatosis type 2 is also called central nervous system neurofibromatosis because of the importance of these related tumors. The central nervous system tumors represent the majority of findings in neurofibromatosis type 2 and vary with the size and extent of the associated tumors.
Acoustic neuromas (vestibular schwannomas) are the most common and well-recognized feature. If bilateral, they are considered pathognomonic of type 2 neurofibromatosis. Patients present with symptoms of tinnitus, gradual hearing loss, and later growth produces brainstem compression, hydrocephalus, and facial palsy.
Spinal cord schwannomas, particularly dumbbell-shaped, are common. Spinal cord ependymomas, astrocytomas, and meningiomas can occur less frequently. Intracranial meningiomas are frequent and can manifest with or without symptoms. Nonvestibular schwannomas, particularly of cranial nerves 3 and 5, are diagnosed at a fairy early age, but can be indolent and slow growing.
Management
Patients with neurofibromatosis type 2 should have annual ophthalmic, neurologic, dermatologic, and auditory examinations. This requires a multidisciplinary team. Surgical resection of symptomatic neurologic tumors is performed, but radiotherapy or chemotherapy can be used, particularly for ependymomas.
Erlotinib has been used for unresectable progressive vestibular schwannomas and this medication is under trial. Additionally, bevacizumab and Gleevec have been investigated for treatment of schwannomas. Regarding ophthalmic care, cataract surgery can be beneficial. Additionally, monitoring of epireticnal membrane with clinical examination and optical coherence.
See also:
- Riccardi VM. (1992) The prenatal diagnosis of NF-1 and NF-2. The Journal of Dermatology 19(11):885–91.
- DiFrancesco JC, Sestini R, Cossu F, et al. (2014) Novel neurofibromatosis type 2 mutation presenting with status epilepticus. Epileptic Disorders: International Epilepsy Journal with Videotape 16(1):132–7.
- Morrow KA, Shevede LA. (2012) Merlin: the wizard requires protein stability to function as a tumor suppressor. Biochimica et Biophysica Acta 1826(2):400–6.
- Ruggieri M, Pratico AD, Serra A, et al. (2016) Childhood neurofibromatosis type 2 (NF2) and related disorders: from bench to bedside and biologically targeted therapies. Acta Otorhinolaryngologica Italica 36(5): 345–67.
- Subbiah V, Slopis J, Hong DS, et al. (2012) Treatment of patients with advanced neurofibromatosis type 2 with novel molecularly targeted therapies: from bench to bedside. Journal of Clinical Oncology: Official Journal of the American Society of Clinical Oncology 30(5):e64-8.

