Pseudoxanthoma Elasticum (PXE)
Clinical Features, Genes and Therapeutics
|
Pseudoxanthoma Elasticum (PXE) (also called Grönblad-Strandberg Syndrome) is a hereditary disorder of the connective tissue that involves the skin, blood vessels, and eyes. |
The pathogenesis of PXE occurs from a dominant gene mutation (MRP6 at 16p13.1), which results in early calcification of elastic fibers. This causes fragmented elastic fibers in the skin, eyes and arteries. It is divided clinically into autosomal dominant Opens in new window types I and II, and autosomal recessive Opens in new window types I, II, and III.
A linear or reticular pattern of small, yellowish papules develops before the age of 30 and may become confluent on the neck, the area below clavicles, and the axilla. Myocardial infarction is the most common cause of death. One should also note that there is an increased risk to mothers during pregnancy (including congestive heart failure and gastrointestinal bleeding).
PXE affects all arteries by the age of 30, causing intermittent claudication, diminished peripheral pulses, and narrowing or occlusion of the peripheral, visceral, and coronary arteries. By age 30, many patients have hypertension and epistaxis.
Skin Features
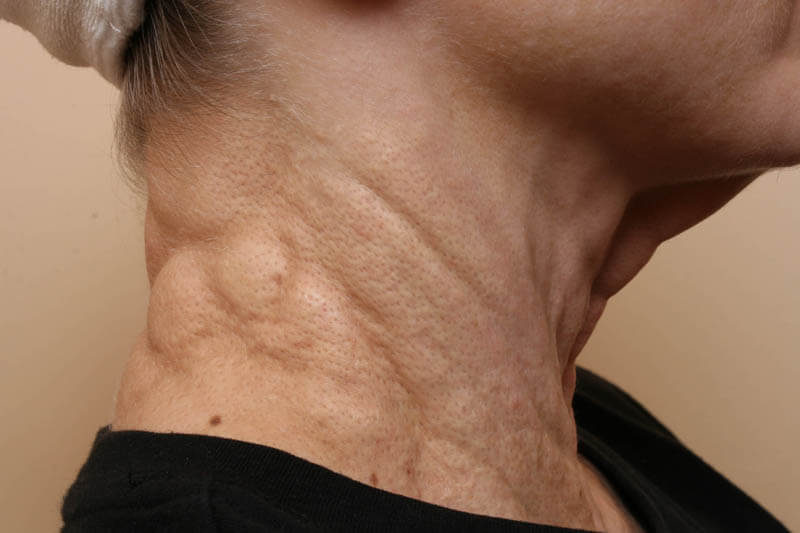
Clinically, PXE is a disease characterized by skin lesions that appear as closely grouped clusters of yellowish papules or plaques arranged in a reticular pattern on the neck, the area below clavicles, and the axilla.
The skin of elderly patients is usually soft, is loose, and hangs in folds, giving a plucked chicken appearance at the neck and axilla. The buccal mucosa may show discrete and confluent small pale yellowish macula-papules.
The lesions are said to have a peau d’orange surface pattern. Yellow papules can also be seen on the mucous membranes such as the soft palate and labial mucosa. Vascular effects include frequent gastrointestinal hemorrhage and early-onset hypertension.
Ocular Features
Retinal hemorrhage and angioid streaks (slate-gray or yellowish streaks appearing wider than blood vessels) represent focal breaks in Bruch membrane. Angiod streaks, named for their resemblance of blood vessels, are often seen on a fundus examination and can lead to blindness.
Usually appearing in PXE patients during the third and fourth decade, the streaks are deep to the retinal vessels and commonly radiate outward from the optic nerve head. The association of the classic skin lesions of PXE with angioid streaks is called the Grönblad-Stranberg syndrome.
Other ocular findings include small retinal and optic nerve head drusen, speckled yellowish mottling of the posterior pole, and subretinal neovascular membranes, which, if near the macula, can lead to severe loss of vision.
Diagnosis
Diagnosis occurs via skin lesions. Biopsy of a scar can detect characteristic changes. Elastic fibers appear curled and “chopped up” with calcium deposition on biopsy. X-ray displays extensive calcification of the peripheral arteries.
Angioid streaks are also characteristic. Special attention should be paid to vascular disease CAD, peripheral vascular disease, and hypertension.
Treatment
Genetic counseling is the mainstay of treatment. Regular reevaluation by primary care physician, cardiologist, and ophthalmologist is mandatory.

