Erythema Dyschromium Perstans (Ashy Dermatosis)
Medical Definition and Introduction
|
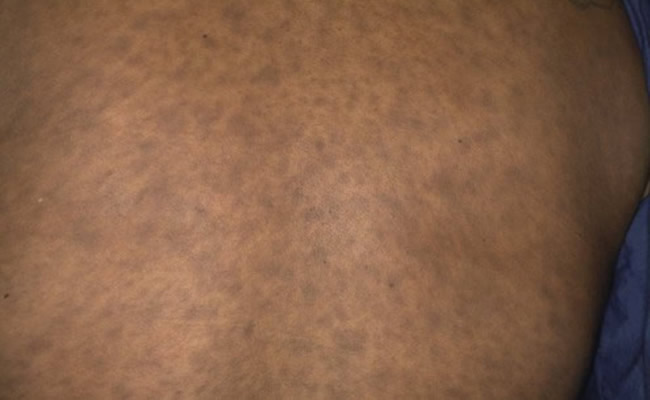
Erythema dyschromicum perstans (also called dermatosis cenicienta, ashy dermatosis) is an acquired, usually asymptomatic, slowly progressive disfiguring hyperpigmented macules on the trunk and proximal extremities, which occurs particularly in Latin American (especially Mexican) populations and in Asians. |
Erythema Dyschromium Perstans (EDP) is an unusual cutaneous eruption was first described in 1957 by C. Oswaldo Ramirez of San Salvador, El Salvador, who referred to patients with this disease as Los cenicientos, which is Spanish for the ashen ones.
EDP was later named dermatosis ceniciento which directly translates to ashy dermatosis. This name refers to the blue-gray hyperpigmented macules that characterize the disease.
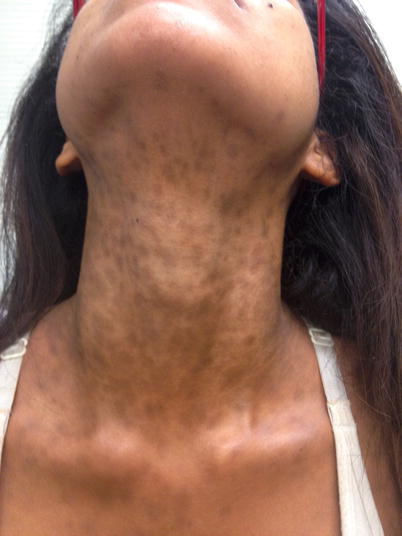
These hyperpigmented macules usually erupt on the face, neck (as seen in the image), trunk and arms as oval, polycyclic, or irregularly shaped.
At onset the macules appear gray in color with an occasional erythematous or elevated border. There are no known systemic symptoms or associations.
Epidemiology
EDP affects males and females equally in a wide range of age groups and has been reported around the world.
Adult EDP more commonly occurs in the second and third decades of life, especially in darker-skinned adults with a Hispanic background, whereas prepubertal EDP occurs more often in Caucasians.
Etiology
The etiology of ashy dermatosis is not clearly known; however, several theories abound. Some authors consider it to be a variation of lichen planus actinicus Opens in new window.
Other authors have considered the geographic distribution of EDP and suggested environmental factors as the etiology.
There have been reports of association with intravenous X-ray contrast media, exposure to pesticides, and whipworm infection in HIV patients.
Oral ingestion of ammonium nitrate, ethambutol, penicillins, and benzodiazepines and contact with chlorothalonil, a fungicide, have also been associated with EDP.
One possible pathomechanism is an abnormal immune response to MHC class II molecules (HLA-DR) and intercellular adhesion molecules.
A study was published in 2007, in which histocompatibility complexes in Mexican Mestizo patients were analyzed. Researchers found that HLA-DR4 was the most commonly associated complex in individuals with EDP, 65% versus 23% for a control group, which lends credence to a genetic etiology.
Clinical Features: Distribution and Arrangement Pattern
EDP can present as blue-gray macules with an active erythematous border, most commonly located on the trunk and proximal extremities and less commonly on the neck and face.
Over time, the patches progressively increase in number and lose their active borders, presenting as symmetrically distributed ashy-gray to blue-brown patches with ill-defined borders.
The patches often present as circular, oval, or polycyclic lesions that spare the palms, soles, scalp, nails, and mucous membranes. EDP is occasionally pruritic but is usually asymptomatic.
Natural History and Prognosis
EDP is a chronic disorder with insidious onset. It often starts as small pigmented macules with a diameter of a few millimeters, but gradually increases in number and size over a period of a few weeks extending peripherally to form converging patches.
In children, these hyperpigmented patches are more likely to resolve over time compared to their adult counterparts.
Differential Diagnosis
The differential diagnosis of EDP as with many pigmentary disorders, includes a drug eruption Opens in new window. A detailed history must be taken to identify concomitant medications. A biopsy will distinguish between a lichenoid drug eruption.
The most frequent pigmentary disorder which can be confused with EDP is lichen planus pigmentosus (LPP) Opens in new window, which can also mimic EDP histologically. However, LPP presents as brownish-black macules or patches without active borders in flexural folds and exposed skin, whereas EDP has erythematous borders in early lesions and prefers sun-protected areas.
EDP can also resemble late pinta Opens in new window, Addision’s disease Opens in new window, melasma Opens in new window, confluent and reticulated papillomatosis Opens in new window, hemochromatosis Opens in new window, and macular amyloidosis Opens in new window, all of which have characteristic findings distinguishing them EDP.
Therapeutics
There is no established therapy for EDP. Many treatments have been attempted, including hydroquinone Opens in new window, topical steroids, antibiotics, griseofulvin, and tretinoin; however, few have been effective. The use of lasers has also been suggested but not proven.
Clofazimine Opens in new window and dapsone Opens in new window may have a beneficial effect on EDP. Clofazimine’s clinical efficacy may be attributed to its tendency to pigment the skin overall, thus obscuring the lesions of EDP.
It may also work through its and anti-inflammatory actions, which have been reported to cause a noticeable decline in the expression of an inflammatory adhesion antigen and major histocompatibility complex class II molecules (HLA-DR).
Dapsone’s efficacy may be due to its ability to suppress neurtrophilic and lymphocytic inflammation and regulate immune responses, although its efficacy is still disputed.
See also:
- Ramirez CO. Los cenicientos: problema clinic. In: Proceedings of the First Central American Congress of Dermatology, San Salvador, December 5 – 8, 1957;122 – 30.
- Silverberg NB, Herz J, et al. Erythema dyschromicum perstans in prepubertal children. Pediatr Dermatol. 2003; 20:398 – 402.
- Tlougan BE, Gonzalez ME, et al. Erythema dyschromicum perstans. Dermatol Online J. 2010;16(11):17.
- Schwartz RA. Erythema dyschromicum perstans: the continuing enigma of Cinderella or ashy dermatosis. Int J Dermatol. 2004; 43:230 – 2.
- Baranda L. Torres-Alvarez B, et al. Involvement of cell adhesion and activation molecules in the pathogenesis of erythema dyschromicum perstans (ashy dermatitis): the effect of clofazimine therapy. Arch Dermatol. 1997; 133:325 – 9.
- Bahadir S, Cobanoglu U, et al. Erythema dyschromicum perstans: response to dapsone therapy. Int J Dermatol. 2004;43:220 – 2.
- Torrelo A, Zaballos P, et al. Erythema dyschromicum perstans in children: a report of 14 cases. J Eur Acad Dermatol Venereol. 2005:19(4):422 – 6.
- Vasquez-Ochoa LA, Isaza-Guzman DM, et al. Immunopathologic study of erythema dyschromicum perstans (ashy dermatosis). Int J Dermatol. 2006;45:937 – 41.

