Intradermal Nevus
Clinical Definition
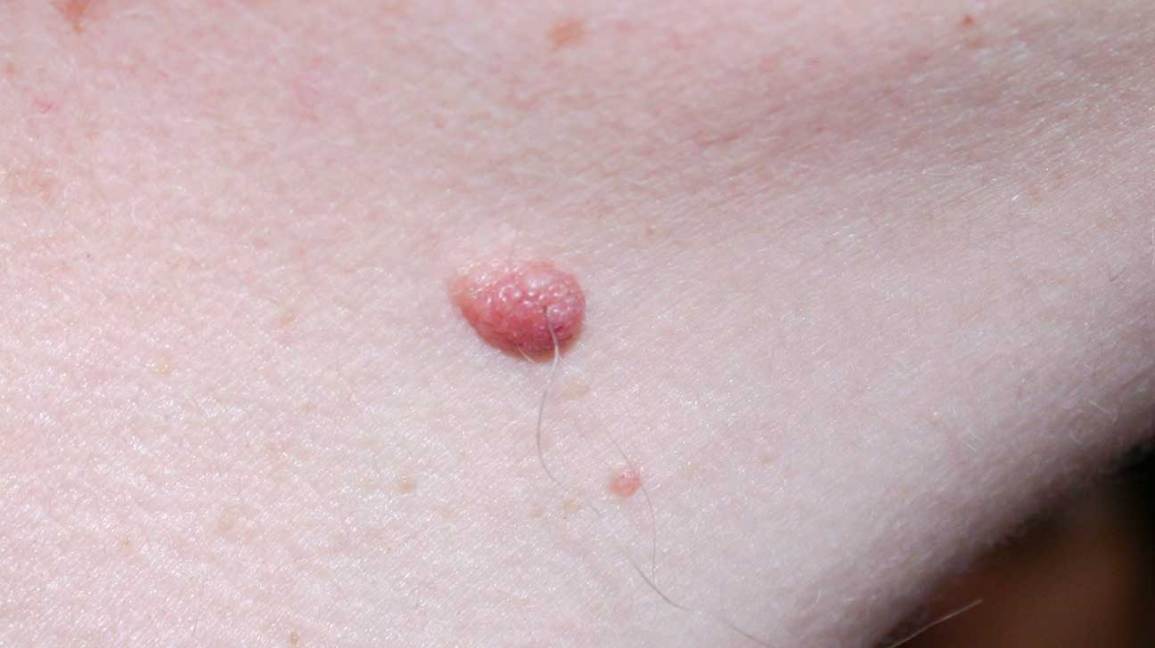 Figure X-1: Intradermal nevus presented in a patient | Photo courtesy of healthline Opens in new window
Figure X-1: Intradermal nevus presented in a patient | Photo courtesy of healthline Opens in new windowIntradermal nevus is generally a small (up to 6 mm) well-circumscribed, hairy papule with generally uniform pigmentation from skin-colored to tan to various shades of brown. The surface may be smooth or rough.
The cells content in intradermal nevi are entirely restricted in the dermis. By definition a significant junctional component is lacking or inconspicuous. Increased numbers of single melanocytes at the junction can be present, but they never aggregate in distinct nests.
In a vast number of cases of intradermal nevi, serial sections will reveal a few small junctional nests, so the distinction between dermal and compound nevus is artificial.
From a biological point of view the cells of an intradermal nevus are in a phase of quiescence.
Clinical Features
Clinically, intradermal nevus is indistinguishable from the compound variant (of which it can be a further evolution). Basically, a dermal nevus can be flat, papillated or nodular.
As in the their compound counterparts these lesions can be named as flat (probably late Clark), Unna and Miescher nevi. The clinical aspect is usually innocent and they are excised only mostly as a cosmetic measure.
Histological Features
Intradermal nevus has the general architecture of the compound variant, the only difference being the loss of the junctional component. General features of these nevi are:
- nested pattern;
- banal, innocent looking cytological features;
- abundance of mature collagen;
- presence of large hamartomatous-looking terminal hair follicles.
Occasionally, the follicular component is complex enough to simulate a tricofolliculoma or a nevus sebaceous. Follicular cysts are also frequent; some papillomatous nevi have induction of sebaceous lobules; - “maturation” in the deepest part of the lesion where smaller and spindle shaped melanocytes are prevalent. Complete neural metaplasia can also be possible, often accompanied by adipocytes;
- absent or inconspicuous mitotic figures.
Differential Diagnosis
As a rule, an intradermal nevus does not pose any differential diagnosis. Occasionally however, the presence of atypical nuclei can create confusion with nevoid melanoma.
In nevoid melanoma however, there are details which are absent in an intradermal nevus with atypical cells:
- atypical cells are prevalent throughout the neoplasm;
- melanocytes have a thickened nuclear membrane with coarse chromatin, the nuclear membrane is of indented and irregular thickness; nucleoli are evident and prominent also in small cells;
- besides atypia there are also numerous mitoses (one or two mitotic figures can be accepted in an otherwise banal intradermal nevus).
The nodular pattern of melanoma is also among the differential diagnoses, for this entity can be completely devoid of any junctional component; however, the distinction is simple; the nodular pattern of melanoma has a strikingly atypical cytology with plenty of mitoses and melanocytes in necrosis.
Other differential diagnoses include glomus tumor, cellular neurothekeoma and neurofibroma.

