Melasma
Medical Definition and Introduction
|
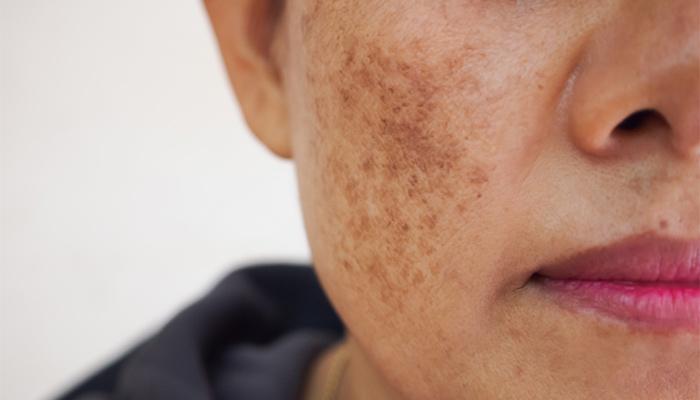
Melasma, a term derived from the Greek melas meaning black, (also known as Chloasma or mask of pregnancy) is an acquired hyperpigmentation of the skin, characterized by blotchy, irregularly patterned, brown or grey-brown symmetrical patches, seen predominantly in women on the areas of the face exposed to the sun, but occasionally on the neck and forearms. |
Most patients are pregnant women in whom the darkening is considered physiologic, although nonpregnant women taking oral contraceptives or estrogens can also develop melasma.
Although women of all ethnic groups are equally affected, melasma appears to be far more prevalent in darker-skinned persons of Hispanic, Oriental and Indo-Chinese origin who live in places with strong solar radiation.
People, especially women of these origins, tend to develop melasma at a rather young age. Melasma may also affect men of these origin. Etiology of the disease is not clearly understood but attributable to sunlight and genetic predisposition.
Etiology
The cause of melasma is unknown. However, many factors have been implicated in the etiopathogenesis of this disease.
Natural and synthetic estrogen and progesterone hormones have been incriminated for its pathogenesis. This is due to the association of the disease with pregnancy, oral contraception and ovarian tumors.
Extensive endocrinological measurements in female patients with melasma, revealed increased levels of luteinizing hormone (LH) and lower levels of serum estradiol, abnormalities suggesting subclinical evidence of mild ovarian dysfunction.
Male patients with melasma have also been shown to have an abnormal hormonal profile with increased levels of circulating LH and low serum testosterone levels.
Although the mechanism of estrogen in precipitating melasma is unknown, it has been reported that melanocytes contain estrogen receptors that stimulate these cells to become hyperactive.
The use of cosmetics with certain components (oxidized linoleic acid, salicylate, citral, preservatives, etc.) and the use of certain drugs (antiseizure, etc.) and photosensitizing agents are often implicated as etiological factors.
As mentioned in the introduction phase, the two most important causative factors are sunlight and genetic predisposition. The role of solar radiation is of great importance.
Exacerbations of melasma are almost inevitably seen after uncontrolled sun exposure and conversely melasma has been seen to fade during periods of sun avoidance.
Genetic and racial factors appear to predominate as suggested by familial occurrence and the fact that the disease is far more common in people of Hispanic, Oriental and Chinese origin.
Clinical Features and Course
Melasma presents as light brown to dark muddy brown or gray-brown macules and patches on sun-exposed areas of the skin.
The number of hyperpigmented patches may range from one single lesion to multiple patches located usually symmetrically on the forehead, cheeks, dorsum of the nose, upper (moustache-like melasma), chin and occasionally on the V-neck area. Melasma does not involve the mucous membranes.
According to the distribution of lesions, the following three clinical patterns of melasma are recognized: the centrofacial, the malar and the mandibular pattern.
- The centrofacial pattern is the most common, observed in about two-thirds of affected individuals, and manifests as lesions on the forehead, nose, upper lip, chin, and medial cheeks.
- The malar pattern consists of lesions on the cheeks and nose, and
- the mandibular pattern is characterized by lesions on the ramus of the mandible.
Individuals often exhibit a mixed pattern of distribution. Melasma has also been observed on the neck and arms; and typically lacks associated symptoms or systemic findings.
Histopathological Features
Histologically, melasma can be classified into three types: epidermal, dermal and mixed. The histological type of melasma can be detected with Wood’s light examination.
- The epidermal type is characterized by intensification of the color contrast between the melasma and the normal skin.
- In the dermal type, the pigmentation of the epidermis is not intensified under Wood’s light and the contrast between the lesions and the uninvolved skin becomes less apparent.
- In the mixed type some areas become more apparent while others become less apparent under Wood’s light in the same individual.
The prognostic significance of this classification is very important to the beneficial effects of the treatment.
Patients with epidermal type respond much better to the use of depigmenting agents. In the case of dermal melanin depositions, elimination of pigment is governed by transport via macrophages and is not accessible to depigmenting agents.
Prognosis
Melasma usually persists for several years. It may present as odd streaking on the face, causing cosmetic disfigurement.
Pregnancy-related melasma may persist for several months after delivery, and melasma related to hormonal treatments may persist for long periods after oral contraceptives have been stopped.
Recurrences are common, particularly after repeat exposure to the sun. The response to treatment can be variable, although dermal-type melasma is less responsive than the epidermal type.
The benefits of treatment may not be apparent for many months. Treatment is often unsatisfactory, and has been associated with side effects such as local irritation, scarring, contact dermatitis, and residual patches of lighter color on the skin—known as confetti pigmentation Opens in new window.
Diagnosis and Differential Diagnosis
The diagnosis is clinical. The initial interview with the patient will give all available information (pregnancy, use of oral contraceptives, genetic and racial involvement, response to sun exposure). The use of Wood’s lamp will assist in the classification into the three afore-mentioned histological types. Skin biopsy can be utilized in difficult cases.
The differential diagnosis of melasma includes post-inflammatory hyperpigmentation Opens in new window, solar lentigines, ephelides, drug-induced hyperpigmentation, actinin lichen planus, facial acanthosis nigricans, frictional melanosis, acquired bilateral nevus of Ota-like macules (Hori’s nevus), nevus of Ota, poikiloderma of Civatte, cutaneous lupus erythematosus, photosensitivity reaction, skin infection, and atopic dermatitis. Unlike most of these diagnoses, melasma is not usually associated with inflammation.
Therapeutics
Although melasma is asymptomatic, treatment is important, as this disorder can pose a cosmetic problem that sometimes causes significant emotional suffering.
Treatments should aim to prevent to the development of melasma, to prevent or reduce the severity of recurrence, to reduce the affected areas, improving the cosmetic defect, and to reduce the time to clearance, with the fewest possible side effects.
The time to clearance is important, as current treatments take several months to have any effect. Treatment options for melasma include depigmenting agents, topical retinoids, topical steroids, chemical peels, laser, and light therapies.
Topical combination therapies have been found to be more effective than monotherapy, particularly triple combination therapy consisting of hydroquinone, tretinoin, and fluocinolone acetonide.
Side effects are usually mild and include irritation, dryness, burning, and erythema of the skin. Kojic acid, isopropylcatechol, N-acetyl-4-cysteaminylphenol, and flavonoid extracts have been investigated as hypopigmenting agents but have not been shown to be superior to creams containing hydroquinone.
Chemical peels, laser therapy, and intense pulsed light have been used but yield unpredictable results and also an increased risk of irritation and post-inflammatory hyperpigmentation.
General Therapeutic Guidelines
Most importantly in the treatment of melasma, patients should be encouraged to avoid the sun as much as possible and use broad-spectrum sunscreen regularly, as the melanocytes in melasma are easily stimulated not only by ultraviolet B (UVB) but also by UVA and visible radiation.
The sunscreen must be applied daily both during treatment and when treatment has stopped, throughout the sunny months of the year for an indefinite period. Sunbathing is absolutely contra-indicated as a few minutes of sunbathing can reverse the benefit of months of therapy.
Women, in whom melasma develops during pregnancy, should avoid exposure to sunlight and should use a broad-spectrum sunscreen every day throughout the pregnancy. These patients should have patience because melasma may fade or clear spontaneously within months after pregnancy.
See also:
- Sheth VM, Pandya AG. Melasma: a comprehensive update: part I. J Am Acad Dermatol. 2011;65(4):689-97; quiz 698.
- Kimbrough-Green CK, Griffiths CE, Finkel IJ, Hamilton TA, Bulengo-Ransby SM, Ellis CN, Voorhees JJ. Topical retinoic acid (tretinoin) for melasma in black patients. Arch Dermatol. 1994;130(6):727-33.
- Chan R, Park KC, Lee MH, Lee ES, Chang SE, Leow YH, Tay YK, Legarda-Montinola F, Tsai RY, Tsai TH, Shek S, Kerrouche N, Thomas G, Verallo-Rowell V. A randomized controlled trial of the efficacy and safety of a fixed triple combination (fluocinolone acetonide 0.01%, hydroquinone 4%, tretinoin 0.05%) compared with hydroquinone 4% cream in Asian patients with moderate to severe melasma. Br J Dermatol. 2008;159(3):697-703.
- Bansal C, Naik H, Kar HK, Chauhan A. A comparison of lowfluence 1064-nm Q-switched Nd: YAG laser with topical 20% azelaic acid cream and their combination in melasma in Indian patients. J Cutan Aesthet Surg. 2012;5(4):266-72.
- Salem A, Gamil H, Ramadan A, Harras M, Amer A. Melasma: treatment evaluation. J Cosmet Laser Ther. 2009;11(3):146-50.
- Farshi S. Comparative study of therapeutic effects of 20% azelaic acid and hydroquinone 4% cream in the treatment of melasma. J Cosmet Dermatol, 2011;10(4):282-7.

