Nevus of Ota
Clinical Definition
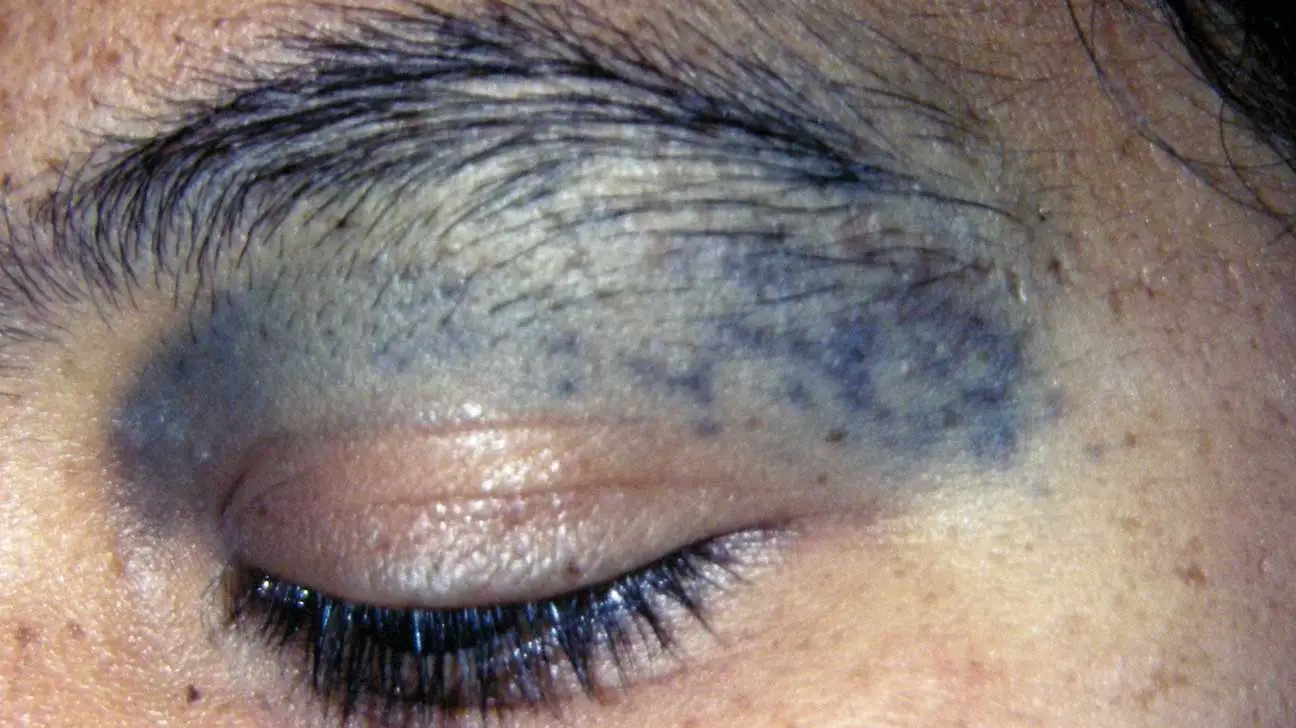 Figure X-1 | Photo courtesy of Healthline Opens in new window
Figure X-1 | Photo courtesy of Healthline Opens in new windowNevus of Ota (nevus fuscoceruleus ophthalmomaxillaris) is a form of dermal melanocytosis Opens in new window described as speckled, irregularly shaped bluish-gray or bluish-brownish macules Opens in new window occurring on the periocular skin (eye area) and sclera (the white outer layer of the eyeball) and, occasionally, the conjunctiva, cornea, and retina.
About two-thirds of patients with this disorder have a patchy bluish pigment or discoloration around the eye, and the surrounding area.
Clinical Characteristics
Clinically, the lesion (or discoloration) consists of large and slightly colored bluish-gray or bluish-brownish macules in the area of the skin which are innerved by the second and third trigeminal branches.
Typically the areas affected include:
- the periorbital region,
- the temple,
- the forehead,
- the malar area (involving the cheek), and
- the nose.
Usually, the lesion is unilateral—involving only one side of the face. Occasionally, it can present bilaterally on both sides of the face—a condition referred to as Hori's nevus Opens in new window.
And in rare instances, the lips, pharynx, and nasal mucosa are similarly affected.
Nevus of Ota is sometimes called nevi of Ota (indicating plurality). Histologically nevi of Ota are indistinguishable from nevi of Ito Opens in new window, except that the latter are found on the shoulder and upper arms as opposed to the face.
|
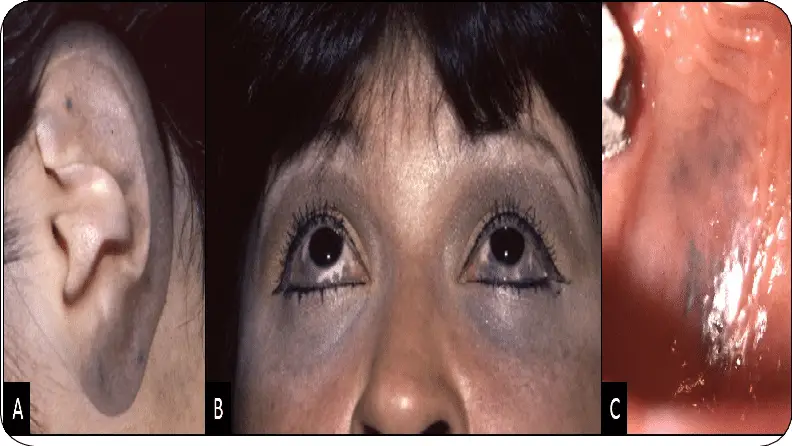
Of note, nevi of Ota are restricted to the skin only in a minority of cases. As a rule, in fact, the lesions involve ocular structures (ocular pigmentation occurs between 22 and 77% of cases according to different studies).
Discoloration involves the sclera, eyelid, choroid and iris; hyperpigmentation of the retina is also possible.
The mucous membranes of the nose, mouth and ear (helix and tympanic membrane) are frequently involved.
In nevus of Ota skin and mucous discolorations are persistent throughout life and do not fade away with time. Color can vary in intensity and the size of the lesion may enlarge.
The incidence of nevus of Ota is common in roughly 0.02% of the Asian population, and nearly 0.2% of Japanese people. It is uncommon in white populations.
There is a strong female predominance. Sixty per cent of nevi of Ota are congenital, but cases of later onset are also possible, especially during puberty. Occurrence in adults or the elderly are very rare.
Disturbingly nevus of Ota has been associated with deafness. Of even more concern, malignant transformations have been reported.
Extra Findings: Association with Other Syndromes
- Association with other dermal melanocytoses.
Nevus of Ota has been described as associated with nevus of Ito Opens in new window.
- Association with ocular lesions.
Nevus of Ota is associated with ocular lesions and can be complicated by glaucoma or cataract (10% of cases). An impaired reflex may be present in the pupil of the affected eye.
- Association with vascular and central nervous system anomalies.
Spinocerebellar degeneration Opens in new window, Sturge Weber disease Opens in new window and Klippel Trenaunay Opens in new window syndromes have been reported in association with nevus of Ota. Also, associations with nevus flammeus Opens in new window and nevus anemicus Opens in new window have been reported.
- Association with extracutaneous and extraocular melanocytoses.
Nevus of Ota can be associated with meningeal melanocytosis Opens in new window, in which melanocytes and pigment are present in the meninges at the base of the skull.
This meningeal involvement is easily associated with black discoloration of the fascia of the temporal muscle.
In nevus of Ota with ocular involvement, pigmentation can also be present in the retrobulbar adipose tissue and the periostium of the orbital bones.
- Melanoma in nevus of Ota.
Melanoma Opens in new window can develop in a nevus of Ota and about 40 of such cases have been reported. The average age of the patient with melanoma is 50 years (15–72) and two thirds are Caucasians. The choroid is the favorite site (but also uveal, iris and optical tract localization is possible); other sites are the central nervous system or other orbital structures and in the skin.
Cases developing in the central nervous system (Balmaceda) are usually correlated with diffuse congenital meningeal melanocytoses of the skull base. As stated above, melanoma in nevus of Ota affects overwhelmingly Caucasians.
Pathogenesis
The etiology of nevus of Ota is presumed to be similar to that of Mongolian spots Opens in new window, involving errors in melanocyte migration from the neural crest to the epidermis
The diagnosis is usually made clinically, based on appearance and location.
Biopsy shows elongated dendritic melanocytes scattered among collagen bundles in the dermis. They are usually more numerous and superficial than in Mongolian spots. At times, melanocytes surround the sheaths of adnexal structures.
Therapeutics
Unlike Mongolian spots Opens in new window, nevus of Ota does not lighten or resolve with time, and may increase in size and color intensity.
An ophthalmologic evaluation is recommended if the periorbital skin is involved, and regular ophthalmologic examinations should be performed if ocular pigment is present.
If desired, treatment with pigmented lesions lasers (e.g. alexandrite or Q-switched ruby) may be considered to help lighten or cause resolution of the lesion, but recurrence after successful laser therapy has been reported.
See also:
- Mishima Y, Mevorah B. Nevus Ota and nevus Ito in American Negroes. J Invest Dermatol. 1961;36:133-54.
- Sekar S, Kuruvila M, Pai HS. Nevus of Ota: a series of 15 cases. Indian J Dermatol Venereol Leprol. 2008;74:125-7.
- Cowan TH, Balistocky M. The nevus of Ota or oculodermal melanocytosis. The ocular changes. Arch Ophthalmol. 1961;65:483-92.
- Landau JM, Vergilis-Kalner I, Goldberg LH, Geronemus RG, Friedman PM. Treatment of Nevus of Ota in Fitzpatrick skin type VI with the 1064-mm QS Nd:YAG. Lasers Surg Med 2011;43:65-7.
- Watanabe S. Takahashi H. Treatment of nevus of Ota with the Q-switched ruby laser. N Engl J Med. 1994;331:1745-50.

