Post-Inflammatory Hypopigmentation
Introduction
|
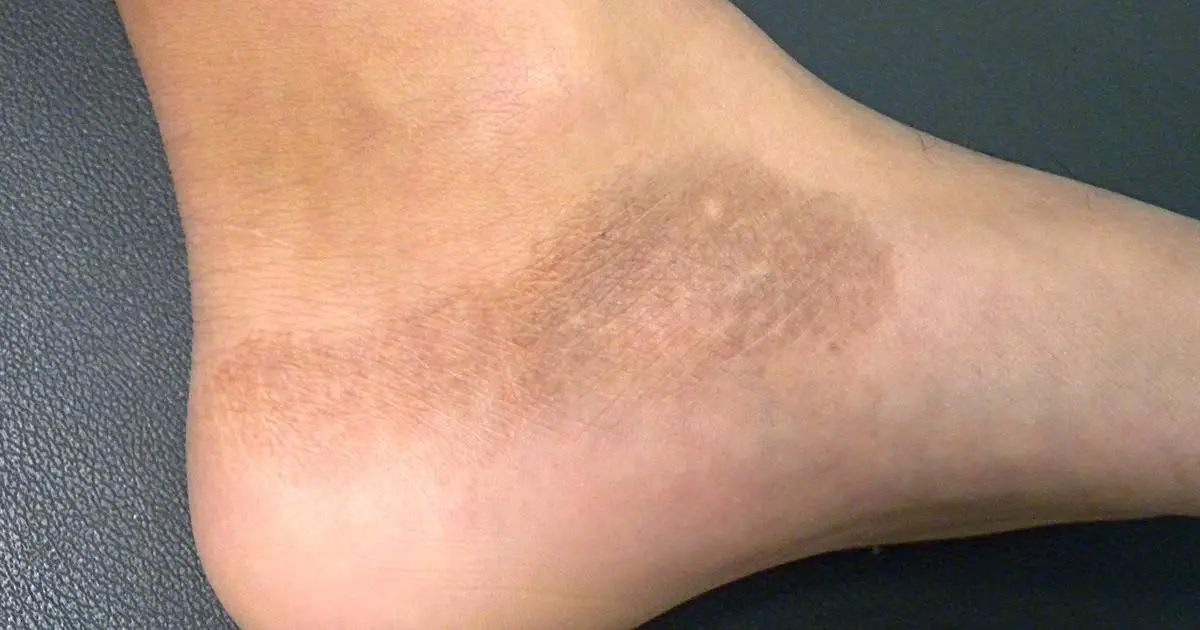
Post-inflammatory hypopigmentation (PIH) is the partial to total loss of melanin following cutaneous inflammation or injury to the skin. PIH is an unfortunate consequence of many dermatologic processes (especially those resulting in inflammation or trauma to the skin). It results from irritated, inflamed or injured skin. |
PIH arises without gender predilection and in all skin types but is more striking and longer lasting in patients with skin of color, where the contrast between the normal and hypopigmented skin may be especially noticeable, often causing significant concern and distress, potentially more so than the condition which preceded it.
PIH has two major etiologies. When inflammation damages the basal keratinocytes, a large amount of melanin is released into the dermis and engulfed by macrophages, creating a characteristic blue-gray color at the site of injury that may be long lasting.
An epidermal response orchestrated by inflammatory mediators such as prostaglandins and leukotrienes causes an increase in synthesis of melanin by melanocytes and subsequent transfer to keratinocytes.
Normal skin pigmentation relies on the production of melanin by melanocytes at the epidermal-dermal junction and the transfer of that melanin to surrounding keratinocytes.
Post-inflammatory hyperpigmentation may be end result of many inflammatory conditions, including allergic reactions, papulosquamous diseases, infections, and burns. In patients with skin of color, however, acne is the most common cause of post-inflammatory pigmentation.
Post-inflammatory hypopigmentation likely reflects alterations to the constitutive melanocyte function by inflammatory mediators, cytokines, and growth factors at the epidermal-dermal junction.
For example, interleukin 1 (IL-1), IL-6, and tumor necrosis factor-alpha (TNF-α) are molecules produced during common inflammatory dermatoses which have been demonstrated to inhibit proliferation and melanogenesis by human melanocytes in vitro.
The response of an individual’s melanocytes to the chemical milieu at the epidermal-dermal junction may be genetically determined.
Clinical Features
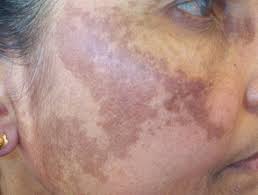
Generally, the lesions of post-inflammatory hypopigmentation are circumscribed macules Opens in new window or patches with sharp to feathered margins (as depicted in the image above). Additional clinical features such as the color, distribution, and arrangement of lesions corresponds to the type and severity of the inciting cutaneous disorder.
For example, mild atopic dermatitis Opens in new window may be followed by slightly hypopigmented lesions, whereas complete loss of pigmentation often occurs in patients with discoid lupus erythematosus Opens in new window. Likewise, the distribution and arrangement of these lesions depend on the configuration of the original inflammation or trauma.
The post-inflammatory hypopigmentation of psoriasis Opens in new window, for example, takes the shape, distribution, and arrangement of the psoriasis lesions. Similarly, post-inflammatory hypopigmentation secondary to lichen striatus Opens in new window appears in the same linear distribution as the primary inflammatory disorder.
Depending on the original condition, the loss of pigmentation may become evident during the active inflammatory or over weeks to months following its resolution. Despite the significant cosmetic and psychological concerns associated with post-inflammatory hypopigmentation, the lesions themselves are typically asymptomatic.
Natural History and Prognosis
The clinical course of post-inflammatory hypopigmentation is largely dependent upon the inflammatory or traumatic process which preceded it.
In most cases, the natural history of the lesions is characterized by improvement with time, especially when the primary process is promptly identified and treated.
For example, post-inflammatory hypopigmentation due to mild atopic dermatitis Opens in new window may resolve within weeks to months, whereas cutaneous inflammation caused by discoid lupus erythematosus Opens in new window may leave severe hypopigmentation which may take years to resolve.
Exposure to ultraviolet radiation Opens in new window, natural or artificial, can hasten repigmentation of lesions. When the inciting cutaneous inflammatory results in irreversible loss of melanocytes Opens in new window, the post-inflammatory hypopigmentation can be permanent.
Pos-inflammatory hypopigmentation can also be a complication of dermatologic procedures, including cryotherapy Opens in new window, laser resurfacing Opens in new window, chemical peels Opens in new window, and dermabrasion Opens in new window.
Histopathological Features
Biopsy of lesions Opens in new window may be helpful in the diagnosis of post-inflammatory hypopigmentation. Histopathological specimens of the hypopigmented lesions typically demonstrate decreased melanin Opens in new window in the epidermis Opens in new window.
Other nonspecific findings may include the presence of melanophages Opens in new window in the upper dermis and inflammatory infiltrate at the epidermal-dermal junction Opens in new window. Additional histopathological evidence, when present, may be useful for determining the preceding clinical condition.
Diagnosis and Differential Diagnosis
The diagnosis of post-inflammatory hypopigmentation relies on a detailed history, as knowledge of any primary cutaneous disorders, previous therapeutic interventions, and other chemical exposures is crucial for a determination of the cause.
While examination under Wood’s lamp Opens in new window can be a useful diagnostic tool for evaluation of hypopigmented lesions, this may not yield as much diagnostic information in patients with darker skin due to lack of contrast between affected and normal skin.
Confocal laser scanning microscopy Opens in new window can provide additional information about the content and distribution of melanin at the epidermal-dermal junction to determine the cause of the hypopigmented macules.
Biopsy with subsequent histopathological analysis of the hypopigmented lesions and surrounding normal skin is also a valuable aid in diagnosis, especially for excluding sarcoidosis Opens in new window, mycosis fungoides Opens in new window, and leprosy Opens in new window, which may present with hypopigmented macules.
The differential diagnosis of post-inflammatory hypopigmentation includes pityriasis alba Opens in new window, ash leaf macules Opens in new window of tuberous sclerosis Opens in new window, chemical leukoderma Opens in new window from job-related exposures, pityriasis versicolor, vitiligo Opens in new window, previous use of intralesional or potent topical corticosteroids, progressive macular hypomelanosis, leprosy, nevus depigmentosus, extramammary Paget’s disease, mycosis fungoides, and sarcoidosis.
Therapeutics
The identification and treatment of the inciting inflammatory condition are the primary goals in the treatment of post-inflammatory hypopigmentation.
These lesions typically demonstrate improvement with time; however, hypopigmentation may persist long after the underlying condition has been treated, especially in patients with skin of lighter color.
Topical administration of medium-potency corticosteroids Opens in new window and tars is the appropriate first-line therapy to stimulate melanogenesis Opens in new window.
Additional treatment strategies include cosmetic camouflage application, topical or oral psoralen plus UVA light (PUVA) therapy, narrowband UVB photo-therapy (NBUVB), and excimer laser therapy.
Pimecrolimus 1 % cream Opens in new window has been shown to be efficacious in restoring skin pigmentation in a pilot trial of African American patients with post-inflammatory hypopigmentation secondary to seborrheic dermatitis Opens in new window.
Skin grafting Opens in new window can be considered in the treatment of severe cases of post-inflammatory hypopigmentation when there has been complete destruction of melanocytes Opens in new window.
See also:
- Ruiz-Maldonado R. Orozco-Covarrubias ML. Post-inflammatory hypopigmentation and hyperpigmentation. Semin Cutan Med Surg. 1997; 16:36-43.
- Vachiramoon V, Thadanipon K. Post-inflammatory hypopigmentation. Clin Exp Dermatol. 2011;36:708-14.
- Halder RM, Nandedkar MA, Neal KW. Pigmentary disorders in ethnic skin. Dermatol Clin. 2003;21:617-28.
- Halder RM, Nootheti PK. Ethnic skin disorders overview. J Am Acad Dermatol. 2003;48(6 Suppl):S143-8.
- Morelli JG, Norris DA. Influence of inflammatory mediators and cytokines on human melanocyte function. J Invest Dermatol. 1993;100:191S-5.
- Kim NY, Pandya AG. Pigmentary diseases. Med Clin North Am. 1998;82:1185-207.
- Xiang W, Xu A, Xu J, et al. In vivo confocal laser scanning microscopy of hypopigmented macules: a preliminary comparison of confocal images in vitiligo, nevus depigmentosus and postinflammatory hypopigmentation. Lasers Med Sci. 2010;25:551-8.
- Halder RM, Richards GM. Management of dyschromias in ethnic skin. Dermatol Ther. 2004;17:151-7.
- Lopez I, Ahmed A, Pandya AG. Topical PUVA for post-inflammatory hypopigmentation. J Eur Acad Dermatol Venereol. 2011;25:734-46.
- High WA, Pandya AG. Pilot trial of 1 % pimecrolimus cream in the treatment of seborrheic dermatitis in African American adults with associated hypopigmentation. J Am Cad Dermatol. 2006;54:1083-8.

